Written by Dr Gowreeson Thevendran, MBChB (Bristol), MRCS.Ed, Dip. Sports Med.Ed, FRCS.Ed (Trauma & Ortho. ), FAMS (Singapore)
What is Plantar Fasciitis?
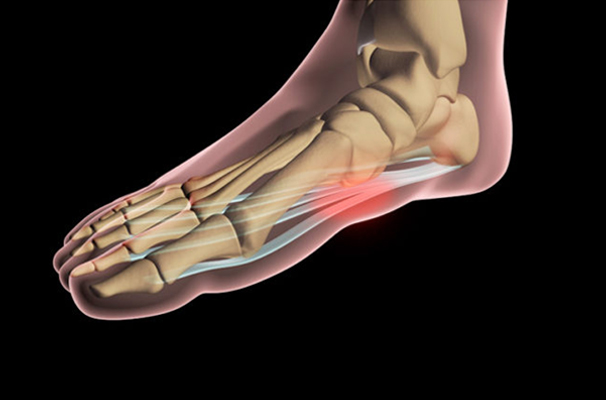
Plantar fasciitis is a condition usually characterised by chronic sharp pain in the heel of the foot. This injury to the plantar fascia, the large, fibrous band of tissue that connects the heel bone to the toes, limits the normal biomechanical functions of the foot. Arch support and shock absorption will also be affected when the plantar fascia tissue is torn or injured. Heel spurs (bony growths in the heel area) may develop as a result of this condition.
Symptoms of Plantar Fasciitis
Pain from plantar fasciitis is usually most acute upon taking your first steps in the morning, after a period of sitting, or after exercise. You may unconsciously find yourself walking on your toes in an attempt to alleviate the pressure from your heel area. If left untreated, plantar fasciitis may develop into a chronic condition. Additionally, you may develop symptoms of other foot and knee injuries, or back strains because the pain from plantar fasciitis can affect the way you walk to compensate for the pain.
Diagnosing Plantar Fasciitis
When diagnosing your condition, if it is indeed plantar fasciitis, your physician will consider your medical history, conduct a physical examination of your foot, and may order additional imaging tests to understand the reasons for your heel pain better. This examination may cover questions about your athletic history, prior or concurrent foot injuries, the specific location and onset of foot soreness, and other aspects of your health and wellness.
A physical examination for plantar fasciitis typically includes the physician applying pressure to the bottom of your feet, bending your toes and foot upward, and considering the shape of your foot. Bone spurs are a common condition associated with plantar fasciitis. X-rays may be ordered to confirm the diagnosis if your physician suspects bone spurs.
Non-Surgical/At Home Treatments For Plantar Fasciitis
Non-surgical treatments for plantar fasciitis include icing, athletic taping, and pain relief medications to ease the inflammation of your condition. Physical therapy, such as stretching and exercise, can also help stretch the plantar fascia and Achilles tendon, which then strengthens the lower leg’s muscles.
For more severe cases, special devices may be needed. They include:
- Night splints: Wearing these splints overnight will hold the plantar fascia and Achilles tendon in a lengthened position to promote stretching
- Orthotics: This custom-made arch support distributes the pressure on your feet more evenly
- Walking boots, canes or crutches: These devices prevent you from moving your foot or placing your full weight on your foot
If the above treatments do not relieve the symptoms, we recommend:
- Injections: Steroid injections provide temporary pain relief. However, multiple shots may weaken your plantar fascia and cause it to rupture. Plasma injections obtained from your own blood can also be considered to promote tissue healing
- Extracorporeal shock wave therapy: Sound waves are directed at the pain area for chronic plantar fasciitis to stimulate healing
- Ultrasonic tissue repair: A probe will be inserted into the damaged plantar fascia tissue using ultrasound imaging. The tip will then vibrate quickly to break up the damaged tissue, which will be suctioned out
- Surgery: If the pain is severe and all other plantar fasciitis treatments fail, surgery will be conducted
Plantar Fasciitis Surgery
Plantar fasciitis surgery, or plantar fasciotomy, aims to alleviate the intense pain associated with plantar fasciitis and correct any underlying issues causing the condition. This surgery targets the plantar fascia, the thick band of tissue that supports the foot's arch, which is essential for foot function and mobility. The surgical approach can be broadly categorised into:
- Open Surgery: Conducted in a hospital, this approach might require general anaesthesia. It involves making a larger incision to access and address the plantar fascia directly
- Endoscopic Surgery: A less invasive method that can be performed in various settings, including hospitals and surgical centres. This option uses local anaesthesia and involves minimal incisions for a quicker recovery
During the Surgery:
- Anaesthesia and Preparation:
- The choice between general anaesthesia and a local anaesthetic with sedative depends on the surgery type. Pre-op instructions will include fasting and medication directives
- Procedure Process:
- Both surgeries are swift, typically concluding within an hour. Open surgery involves a direct approach to the fascia, while endoscopic surgery uses small incisions and a camera to guide the procedure
Recovery Period For Plantar Fasciitis
The recovery experience for plantar fasciitis surgery varies significantly between the open and endoscopic surgical approaches:
General Post-Op Instructions:
- Immediate Aftercare: Instructions will be provided for home care, emphasising keeping the foot elevated to reduce swelling and pain. This also helps in preventing fluid buildup around the surgery site
Recovery from Open Surgery:
- Post-Surgery Care: A walking boot, cast, or special shoe might be necessary for several weeks to aid healing. Stitches or casts will be removed during follow-up visits. Post-surgery care includes wearing a flat Darco sandal for 2 to 3 weeks, followed by trainers to support recovery.
- Healing Time: Full recovery typically spans 6 to 10 weeks, during which normal footwear is gradually reintroduced. Expect a small scar from the incision site
Recovery from Endoscopic Surgery:
- Weight Bearing and Footwear: Limited weight can be placed on the foot shortly after surgery, with a return to regular shoes possible within 1 to 2 days. Scarring is minimal
- Overall Recovery: Advised to limit foot strain for several months. Recovery might include exercises for flexibility and strength, undertaken independently or with a therapist
- Healing Duration: The recovery period is generally shorter, lasting 3 to 6 weeks, dependent on individual healing rates and following doctor's recommendations closely
Follow-Up Care:
- Monitoring Progress: Essential for both types of surgeries to ensure healing is on track and to address any concerns promptly.

Dr Gowreeson Thevendran
MBChB (Bristol), MRCS.Ed, Dip. Sports Med.Ed, FRCS.Ed ( Trauma & Ortho. ), FAMS (Singapore)
Dr Gowreeson Thevendran is an orthopaedic surgeon in Singapore who specialises in lower limb orthopaedic conditions, trauma, and fracture surgeries of both the upper and lower limbs. He received his medical education from the University of Bristol and completed his surgical training in the UK and Canada. Before establishing his private practice, he served as Chief of Foot & Ankle Surgery, Department of Orthopaedics at Tan Tock Seng Hospital, Singapore.
Dr Gowreeson Thevendran’s Qualifications and Awards:
- Bachelor of Medicine and Surgery, University of Bristol, England
- Fellow of the Royal College of Surgeons, Edinburgh
- Diplomate Faculty of Sports and Exercise Medicine, Royal College of Surgeons Edinburgh
- Fellow of the Academy of Medicine, Singapore
- SICOT PIONEER Founders Award 2020
- 2015 European Foot & Ankle Society ‘Best Podium Presentation’ Award
- 2013 Singapore Orthopaedic Association Junior Travelling Fellowship
- 2012 NHG Critical Talent Special Recognition Award
- 1998 Enid Lindt Prize in Clinical Surgery
- 1995 Public Services Department Full Medical Scholarship
Languages Spoken:
- English, Malay, Tamil
COMMON ORTHOPAEDIC CONDITIONS WE TREAT
GENERAL
Frequently Asked Questions About Plantar Fasciitis Treatment in Singapore
For many, plantar fasciitis can be managed effectively with non-surgical approaches. These include the RICE method (Rest, Ice, Compression, Elevation), prescribed anti-inflammatory medications, and physical therapy to alleviate symptoms. Should these conservative treatments not fully address the condition, consulting with a sports injury doctor in Singapore to discuss further options, potentially including surgery, is recommended.
Related posts
Clinic Location
OrthofootMD@Novena
- Mount Elizabeth Novena
38 Irrawaddy Road #05-42 Mount Elizabeth Novena Specialist Centre Singapore 329563
OrthofootMD@Mount Alvernia Hospital
- (Mount Alvernia Hospital)
820 Thomson Road #01-01/02 Mount Alvernia Medical Centre A Singapore 574623
Dr Gowreeson Thevendran is currently an orthopaedic surgeon with Island Orthopaedic, a one-stop care centre for orthopaedic health under Healthway Medical Group. He specialises in treating lower limb orthopaedic conditions, as well as trauma and fracture surgery of both the upper and lower limbs. Prior to establishing his private practice, Dr Gowreeson was Chief of Foot & Ankle Surgery at the Department of Orthopaedics at Tan Tock Seng Hospital (TTSH). Today, he continues to serve the Orthopaedic Department at TTSH as a visiting consultant.