
Will my Torn Hamstrings Spell the End of my Sports Career?
March 2, 2021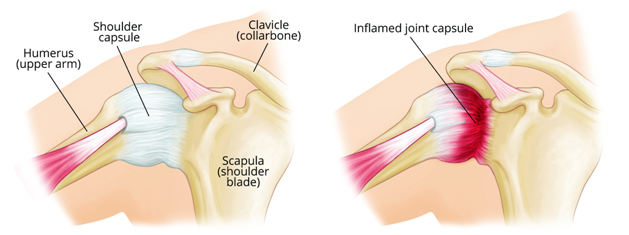
The Wrath of a Frozen Shoulder
March 8, 2021An Overview of Flat Feet
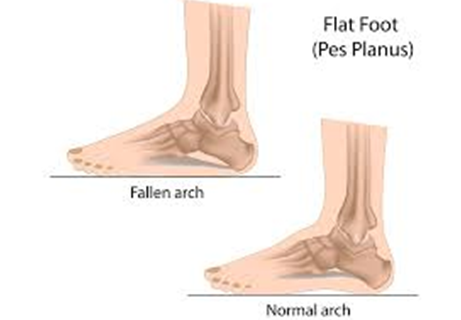
Flat feet is also known as pes planus, a deformity in which the arch of the foot collapses and nears the ground. The deformity could be by birth or it can develop over time in adults. A child is born with flat feet. In infants and toddlers, flat feet is normal becausethe arch of their feet is not developed until they begin walking.
When children grow and start standing on their feet, their muscles develop, and an arch appears in their feet. The arch keeps growing throughout childhood, and when they become adults, the arch is completely developed. But, there are some cases when the arch is not completely developed. For some people, it is normal to have flat feet and they don’t feel any pain at all. On the contrary, there are some cases where people may face problems like pain in the heel or arch area, difficulty in standing and walking, swelling alongside the ankle.
If you want to diagnose flat feet, this requires a physical examination along with the support of medical imaging tests. Almost 30% of the world’s population has flatfeet as a normal variant as part of their development.
Symptoms of a Progressively Flattening foot ….
The symptoms of a progressive flat foot appears gradually. The main symptoms are pain and swelling on the inside or outside of your foot or ankle which increases when you perform any activity. The other symptoms that accompany pain and swelling include a loss of arch, weakness in your feet, inability to stand on your toes, and tenderness in your midfoot, especially when you perform any physical activities.
Causes of Progressively Collapsing Foot
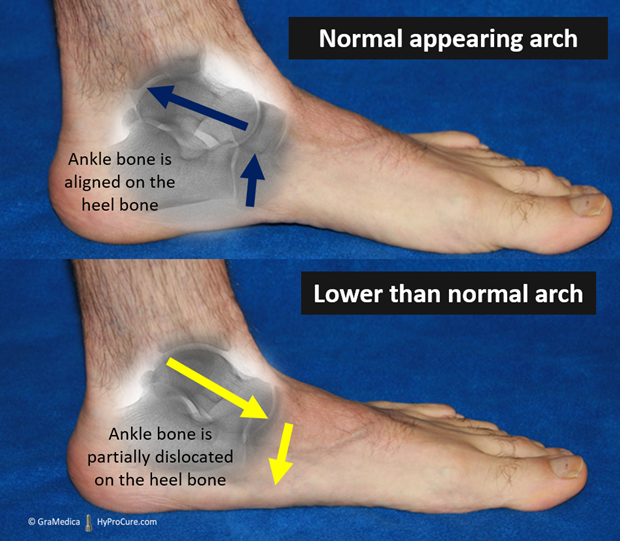
A progressive flatfoot is common after body weight increase, a phase of strenuous physical activity or in cultures wear sandal-wearing is common. Some causes of progressive flatfoot are given below:
- Diabetes
- Obesity
- Injury or Sudden Trauma to the supporting structures
- Inflammatory diseases such as rheumatoid arthritis or psoriasis, etc.
- People that are more actively involved in sports can get tears in their posterior tibial tendons. As a result, they can develop flat feet.
Diagnosing Flat Feet
In most cases, flat feet can be self-diagnosed. However, there are some cases when you need help from a foot specialist to diagnose flat feet. There are two methods used to diagnose flatfeet.
Physical Examination
A foot specialist can diagnose flat feet by looking at your feel and performing various physical tests. Some of the visual tests used for flat feet diagnosis are:
The Wet Footprint Test
In this test, you are asked to stand on a smooth and level surface with wet feet. The thicker the print between the heel and ball of the foot, the flatter the foot is. A normal high arch foot will only leave a thin print on this area.
The Shoe Inspection Test
In this test, your shoe is inspected to look for evidence of faulty foot mechanics. Your shoes will be more worn from the inside if you have flat feet. The upper part of your shoes will also lean inwards towards your sole.
The Tiptoe Test
The tiptoe test is used to check if your flat feet is rigid or flexible. If the arch is visible when you stand, this implies your flat feet is flexible. If not, it could mean you have a rigid flat foot and your doctor will suggest treatments accordingly.
Medical Imaging
If you are having pain in your feet and you are concerned this may be due to flat feet, then your doctor can perform various imaging tests to pinpoint the actual cause of the problem.
X-rays
X-rays are suitable for diagnosing joint arthritis and detecting the irregularities in the alignment of your foot bones.
UltraSound
Ultrasound can be used to get detailed images of tissues ( ligaments & tendons ) to detect ruptures and tears.
Magnetic resonance imaging
MRI is more detailed as compared to x-rays and ultrasound. It gives better image definition and delineation of pathology
What Treatment Options Are Available for the Progressively Collapsing Foot?
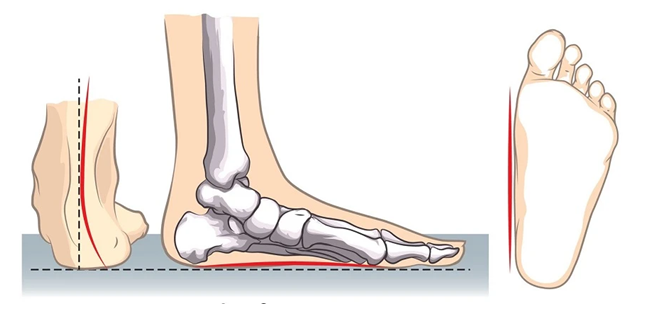
Non Surgical Treatments
In adults, fallen arches usually don’t need any treatment. Those experiencing symptoms can use orthotic arch supports and foot arch strengthening exercises. If you also have pain and swelling in your feet, then you can take NSAIDs, orthotics and even consider a corticosteroid injection.
Orthotic supports are used to change the structure of your feet and bring back their alignment but this could take weeks if not months to achieve. You can also perform some exercises like foot gymnastics, runner’s stretch, and therapeutic massage to increase the arch flexibility and strength of your feet.
Surgical Options
If the pain keeps getting worse and none of the above treatments work for you, then a flat foot reconstructive surgery is the only option to get relief from pain. Your doctor will decide which approach should be used for your surgery depending on different factors like age, symptoms, and the severity of the flatfoot deformity.
Recovering from flat foot surgery could take several months and often requires the patient to be in a walker boot for 6-8 weeks before transitioning into supportive running shoes.
So, if your foot is collapsing progressively, then there is no need to worry. There are plenty of treatment options available that you could explore to make things better. If you want more information regarding these treatment options, please contact Dr. Gowreeson Thevendran or visit: www.orthofootmd.com.



